Abstract: This policy brief raises a concern about the persistently low rates of deworming among pregnant women, as reported through the Health Management Information System (HMIS) data. Deworming using a single dose of Albendazole during the pregnancy is an important component of the package of services under the ante-natal-care (ANC). The adverse effects of worm infestation on morbidity, malnutrition and other peri-natal outcomes are well documented. Yet coverage rates for albendazole remain significantly low compared to distribution of IFA and Ca tablets, both multi-dose, and the Tetanus Toxoid (TT) injection. This ‘coverage deficit’ for deworming service amounts to filling a ‘leaking bucket’. The helminths have the last laugh, notwithstanding the high coverage under other ANC components. It is high time that this deficit is eliminated with all seriousness.
Background: Soil Transmitted Helminths (STH) infections are common worldwide, contributing to a high burden of malnutrition and morbidity in resource poor settings (MoHFW, 2014). More than 1.5 billion people i.e., 24% of the total world population are infected with STH (WHO, 2021), majorly affecting the women in reproductive age, including pregnant women (Zegeye et. al., 2021). Literature suggests that pregnant women with intestinal parasitic infections are at an increased risk of maternal complications and adverse perinatal outcomes like anaemia, low birth weight and perinatal mortality (Ibid). According to the ‘National Guidelines for Deworming in Pregnancy’, up to 41% iron-deficiency anaemia in pregnant women in some populations is attributed to hookworm infestation, which results in higher maternal morbidity and mortality, pre-term births, Intra Uterine Growth Restrictions (IUGR), low birth weight (LBW) and poor iron status in the infant (MoHFW, 2014). A multi country study has documented that the preventive therapy of deworming of pregnant women and children significantly improves the Hb levels and nutritional status (Zegeye et. al., 2021). A study of more than 800,000 births from 95 Demographic and Health Survey (DHS) datasets reveals that when women receive deworming medicine during pregnancy, there is a 14% reduction in the risk of neonatal mortality (Walia et. al., 2021).
Against this backdrop, the recently published National Family Health Survey 2019-20 (NFHS-5) raises concern about the alarming state of anaemia in pregnant women (52.2%) and children (67.1%) under the age of five years. As per NFHS-4 (2015-16), 50.4% pregnant women and 58.6% children under the age of five years were anaemic. The rise in these figures when compared to NFHS-4 (2015-16), raises questions on the efficacy of IFA supplementation during pregnancy and focused intervention on anaemia reduction like ‘Anemia Mukt Bharat’. Likewise, the neonatal mortality rate (NNMR) in India, though reduced to 24.9 (NFHS-5) from 29.5 (NFHS-4), remains well above the global average of 17.47 (UNICEF, 2020), SDG 2030 target of less than 12 and National Health Policy target of less than 16 by the year 2025.
In India, deworming during pregnancy is carried out as per ‘National Guidelines for Deworming during Pregnancy’, (MoHFW, 2014), which suggests one dose of albendazole (400mg) tablet for the pregnant women after first trimester in areas where STH prevalence is greater than 20%. Fig. 1 shows the coverage under different services provided during antenatal care, for the four-year period FY18 – FY21, defined as the percentage number of women covered, compared to those having received four or more ANCs.
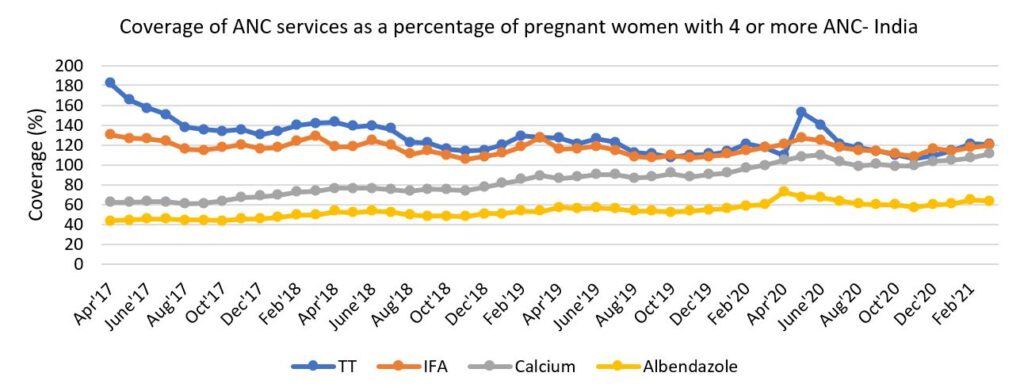
Source: HMIS (FY18 – FY21)
While the unusually high coverage under IFA, Calcium and TT raises questions about the quality of data and the need for de-duplication, the coverage under albendazole for pregnant women does not reach even 65%. Interestingly, the coverage under supplementation of 360 Calcium tablets which was introduced in the same year as albendazole (National Guidelines for Calcium Supplementation during Pregnancy and Lactation, 2014), has improved at a much faster pace than that of albendazole. The TT, IFA and Calcium coverage above 100% in the year 2020-21, means that even the pregnant woman who has less than four ANC visits, has received one TT dose, 180 IFA tablets and 360 Calcium tablets. Yet, easy to comply, single-dose Albendazole tablet remains the step child of the ANC services with all its downstream consequences.
Data consistency of HMIS: Literature suggests that HMIS data might suffer from data duplication or data inconsistency due to misinterpretation of data elements by data entry operators and other systemic issues. To check the consistency of the data across different years, we regress the albendazole coverage data as well as the data on pregnant women with 4 or more ANC for FYs 2018-19, 2019-20 and 2020-21 on the 2017-18 data (Fig. 2 and Fig. 3).
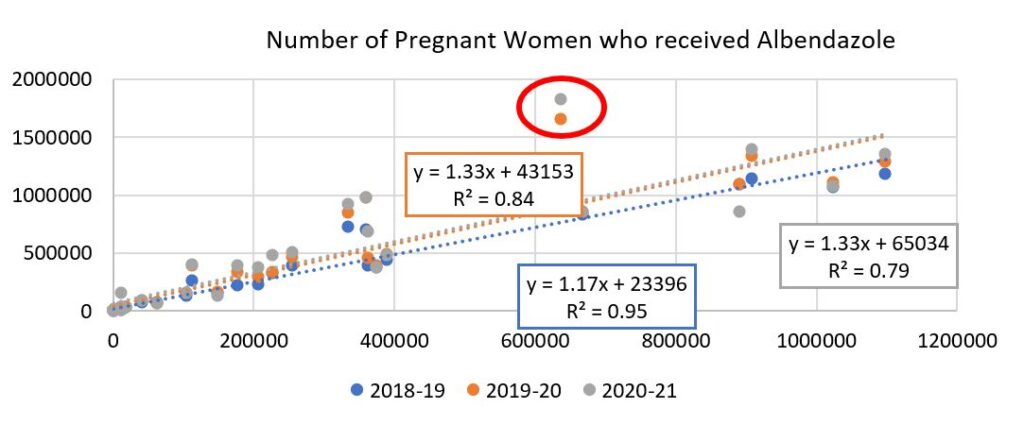
Source: HMIS (FY18 – FY21)
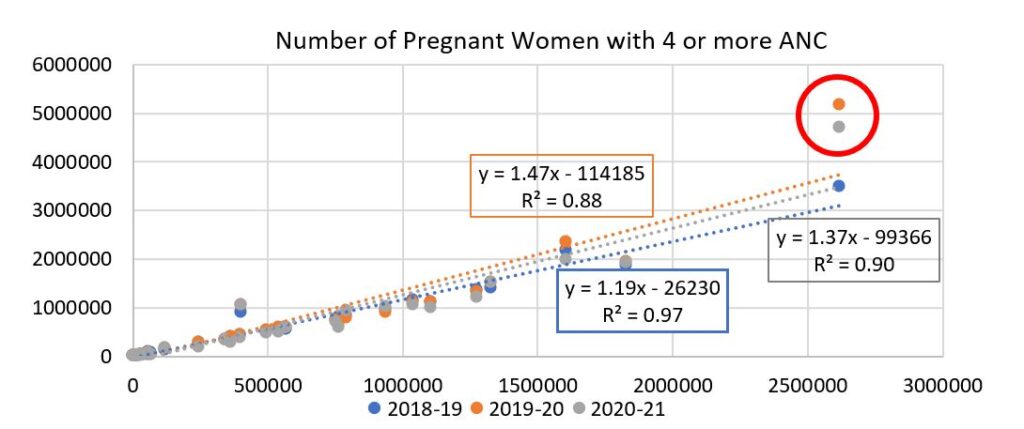
Source: HMIS (FY18 – FY21)
The linear fit, with high R-Square values indicates a fairly consistent reporting across all states, except Uttar Pradesh (circled in red), which emerged as an outlier for both indicators, for the years 2019-20 and 2020-21. The coverage under albendazole, while consistent across the four-year period, also shows considerable regional variation. We analyse the regional patterns next, both at the state level and the district level
Key Findings Based on albendazole coverage from the HMIS Data Analysis
Figure 4 provides the state-wise coverage of pregnant women having received albendazole tablets as a percentage of the women that have received four or more ANC visits for the period 2017-21. There is an evident increase in albendazole coverage, across states, over the four years. The increase during the pandemic year 2020-2021 is particularly significant. It is worth examining whether this was on account of more home visits of the health workers owing to the lockdown and the attendant restriction on movement of the pregnant women. This is also interesting as there has been general disruption of non-Covid services as documented elsewhere (Kumari et al., 2020; Nasta et al., 2020).

Source: HMIS (FY18 – FY21)
While the guidelines for deworming during pregnancy (MoHFW, 2014) stipulate providing one tablet of albendazole to a pregnant woman after her first trimester in all locations where STH infections have more than 20% prevalence, we do not have the latest data on STH prevalence. We use results of the study carried out by GAHI (Global Atlas for Helminth Infections) in the year 2015 (see Figure 5).
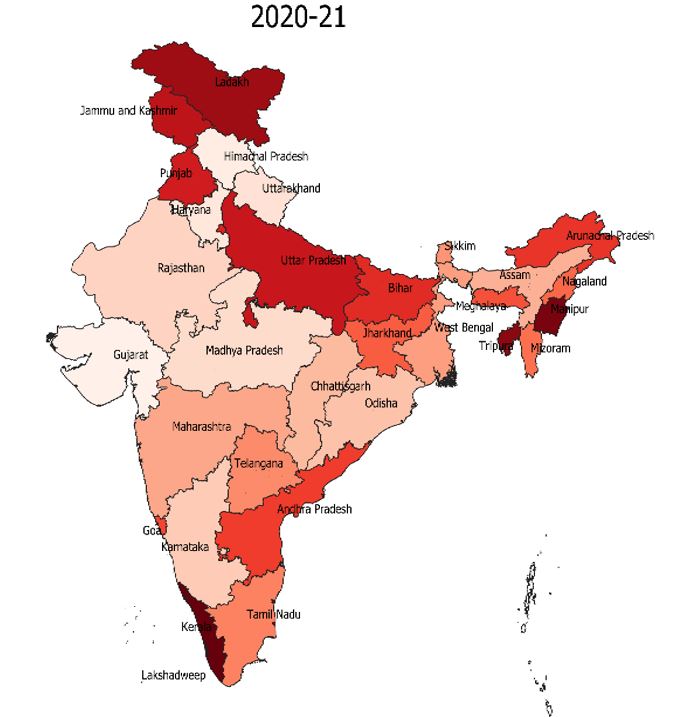
If we compare the above two figures, we see that that Kerala, Bihar, Jammu & Kashmir and the North-Eastern states with high STH prevalence (>20%), are showing low albendazole coverage (darker shades represent lower coverage) in the year 2020-21. The poor albendazole coverage in these states is not confined to just one-year; but is a persistent trend, across the years (see Figure 4). These states need to focus on increasing their albendazole coverage. The case of Kerala with its impressive health statistics otherwise, warrants a more detailed scrutiny.
On comparing the coverage of albendazole with the coverage of one dose of TT, 180 IFA tablets and 360 Calcium tablets, it is seen that in all the states albendazole has the least coverage (Fig. 7). However, the level of difference in coverage of albendazole and other services varies from state to state.
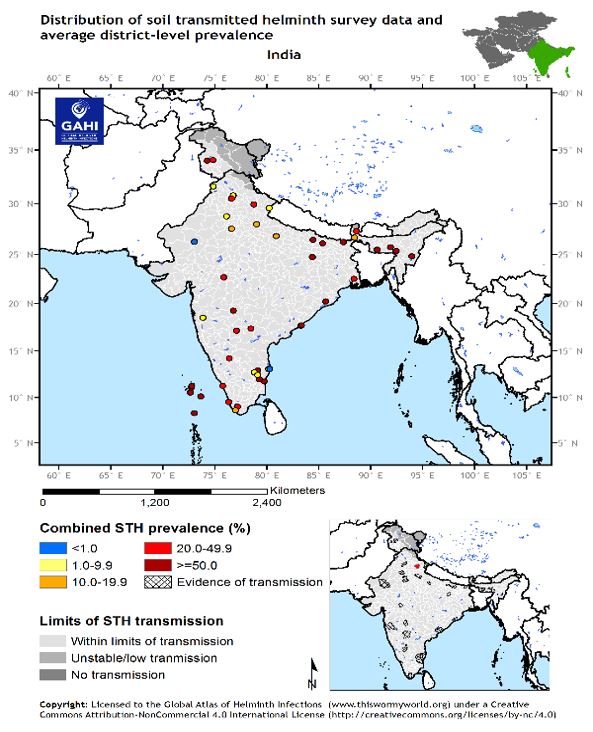
Source: GAHI, 2015
Source: HMIS (FY21)
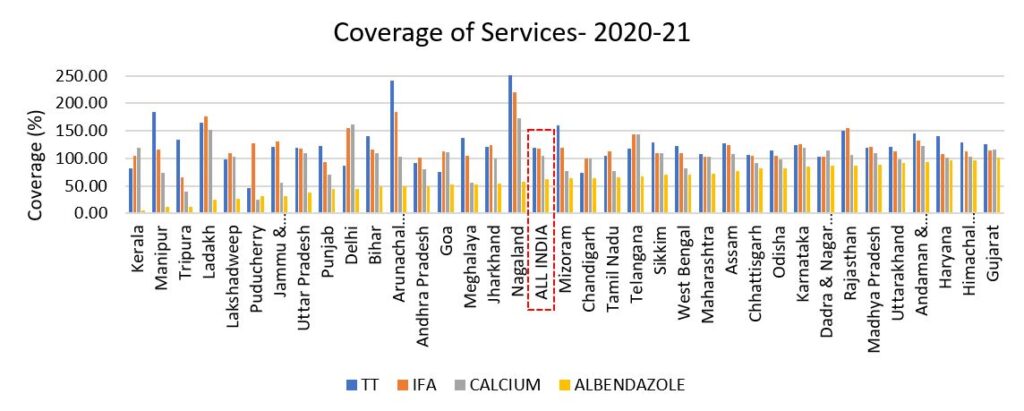
Source: HMIS (FY21)
While states like Gujarat, Himachal Pradesh and Haryana show above 90% coverage of all the services (TT, IFA, Calcium and Albendazole), states like Kerala, Manipur, Uttar Pradesh and Delhi show good coverage (above 80%) for TT, IFA and Calcium supplementation service but a below 50% coverage for Albendazole prophylaxis. A district level mapping of Albendazole coverage is carried out to check whether poor coverage is a result of extremely low coverage in select districts or, or it is a state-wide issue
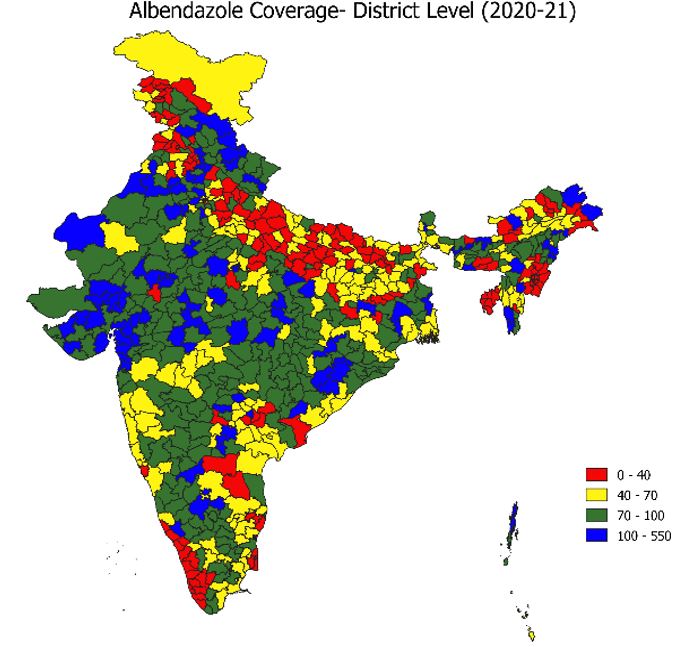
Source: HMIS (2021)
Figure 8 shows that the states with poor coverage as well as high (greater than 20%) STH prevalence, i.e., Kerala, Bihar and Manipur have state-wide problem of low coverage of Albendazole. Table 1 shows the top 10 and bottom 10 districts in terms of Albendazole coverage in the year 2020-21. 106 out of 735 districts i.e., 14.69% districts are reporting more than 100% coverage (highlighted with ‘blue’ colour in Figure 8).
Table 1 Top 10 and bottom 10 districts in terms of Albendazole coverage
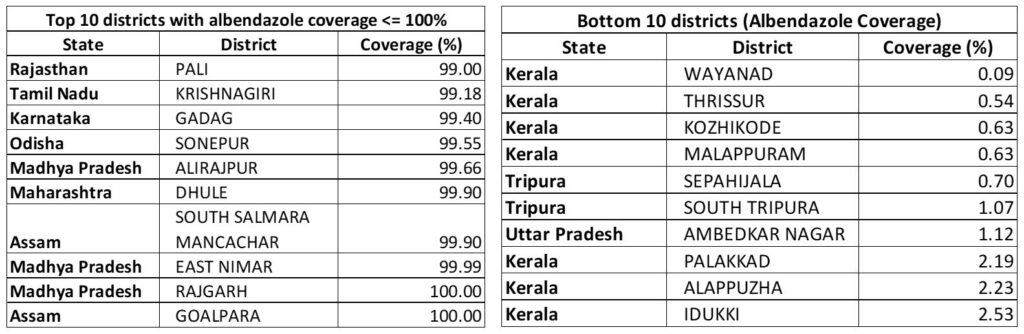
Source: HMIS (2021)
However, the coverage above 100% would warrant a careful examination of the data and its ground truthing in these districts.
While literature highlights (Christian et. al., 2004) the benefits of Albendazole prophylaxis in reduction of NNMR, and in we do not find any correlation between the albendazole coverage and neonatal mortality rates reported in the HMIS. This also the case with the reported anaemia coverage. However, HMIS is not the right data set to assess NNMR. Even for anaemia levels one will need to go to the RCH data of individual mothers given that their Hb level is checked 4 times during pregnancy. However, this policy brief is more about adherence to the prescribed norms of albendazole coverage rather than about determining its efficacy which is subject matter of a separate analysis using RCH data of individual mothers. The case of Kerala where the albendazole coverage is consistently low yet the figures on neonatal mortality as well as anaemia prevalence among pregnant women are low merits a closer scrutiny of the current policy.
Conclusion: The analysis presented above reveals the low levels of Albendazole coverage across the years and across the nation while the other components of the same ANC package i.e. IFA, Calcium and TT, continue to show nearly complete coverage. This is not withstanding the documented benefits of deworming and the adverse impact on the maternal and child health if the worm infestation is not tackled at the right time. This coupled with the persistence of anaemia levels among pregnant women and high neonatal mortality rates is a wake-up call for the health system. It is high time that albendazole coverage should become a strong monitoring item as well as a criterion for the incentives that ASHAs receive.
Authors:
Patel K. R., Agnihotri S. B.
Krritika R Patel (krritikapatel@gmail.com) is has completed her M.Tech in Technology and Development at CTARA, IIT Bombay. Currently, she is a UNICEF-CTARA Fellow.
Prof Satish B Agnihotri is Emeritus Fellow CTARA at IIT Bombay and works, inter alia, on Child Malnutrition, Health and Nutrition Policy.
References
- Christian, P., Khatry, S.K. and West Jr, K.P., 2004. Antenatal anthelmintic treatment, birthweight, and infant survival in rural Nepal. The Lancet, 364(9438), 981-983
- Global Atlas of Helminth Infections. (2015). Distribution of soil transmitted helminth survey data in India. Retrieved from http://www.thiswormyworld.org/maps/distribution-of-soil-transmitted-helminth-survey-data-in-india.
- Kumari, V., Mehta, K., & Choudhary, R. (2020). COVID-19 outbreak and decreased hospitalisation of pregnant women in labour. The Lancet Global Health, 8(9), e1116-e1117
- Nasta, A. M., Goel, R., Kanagavel, M., & Easwaramoorthy, S. (2020). Impact of COVID-19 on General Surgical Practice in India. Indian Journal of Surgery, 82(3), 259-263.
- Maternal Health Division, MoHFW (2014, December). Retrieved from http://nhm.gov.in/images/pdf/programmes/maternal-health/guidelines/National_Guidelines_for_Deworming_in_Pregnancy.pdf
- (2021, April). Retrieved 12 17, 2021, from https://www.who.int/news/item/29-04-2021-deworming-women-during-pregnancy-has-a-positive-effect-on-child-survival-and-health
- Walia, B., Kmush, B. L., Lane, S. D., Endy, T., Montresor, A., & Larsen, D. A. (2021). Routine deworming during antenatal care decreases risk of neonatal mortality and low birthweight: A retrospective cohort of survey data. PLoS neglected tropical diseases, 15(4), e0009282. https://doi.org/10.1371/journal.pntd.0009282
- UNICEF Global Database, as on 09 September 2020.
- Zegeye B., Keetile M., Ahinkorah B. O., Ameyaw E. K., Seidu A., Yaya S. (2021). Utilization of deworming medication and its associated factors among pregnant married women in 26 sub-Saharan African countries: a multi-country analysis. Tropical Medicine and Health.
